Eating Disorder and Substance Abuse Treatment Centers
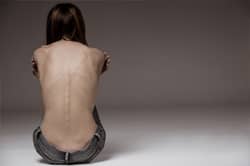 Eating disorders, including anorexia, bulimia, and binge eating disorder, are serious conditions that often become life-threatening. The health effects of eating disorders can become even more severe when substance abuse is added to the mix.
Eating disorders, including anorexia, bulimia, and binge eating disorder, are serious conditions that often become life-threatening. The health effects of eating disorders can become even more severe when substance abuse is added to the mix.
Addiction and eating disorders frequently occur simultaneously. In the United States, 20 million women and 10 million men will struggle with an eating disorder at some point in their lives.2 Researchers estimate that up to 50% of these people abuse alcohol or use illicit drugs.3 In contrast, about 9% of the general population struggles with substance abuse.3
Comorbidity is a term used to describe two or more separate disorders occurring at the same time in one individual. The concept also includes instances in which the separate disorders arise one after the other. Comorbidity, which can also be called a dual diagnosis or co-occurring disorder, implies that the combination of illnesses can worsen the course of both. It follows that, in most cases, both conditions must be treated for the person to fully recover.
Addiction and Eating Disorders
Addiction and eating disorders go hand in hand because people that have eating disorders often use drugs and alcohol to suppress appetite, boost energy, and promote weight loss.3
People with eating disorders often abuse the following:3
- Caffeine
- Tobacco
- Alcohol
- Amphetamines
- Cocaine
- Heroin
- Diuretics
- Ipecac syrup
- Laxatives
It goes the other way, too. People with substance abuse disorders are far more likely than other people to develop an eating disorder. Around 3% of the general population is struggling with an eating disorder, but among alcoholics and drug abusers, the number is closer to 35%.3 Bulimia and alcohol abuse are often seen in the same person, as is anorexia and substance abuse.
The relationship between bulimia and alcohol abuse is the strongest of the associations.
Alcoholism is extremely common in women with eating disorders, and its prevalence is much higher than that found in the general population. Conversely, women who struggle with alcoholism are more likely than other women to develop symptoms of an eating disorder.3
The relationship between bulimia and alcohol abuse is the strongest of the associations. This is a dangerous combination, as it has been associated with higher rates of suicide attempts, anxiety disorders, and personality disorders than seen in bulimic women without alcohol dependence.3
Eating disorders and alcohol abuse are major concerns in pre-adolescent and early adolescent girls. Girls in this age group who express significant worries about their weight are nearly twice as likely than other girls to begin getting drunk.3 Conversely, girls who have a history with drinking and drunkenness are approximately 3 times more likely to begin purging for weight control.3
Effects
 Eating disorders and substance abuse have many serious health consequences. The following is a list of potential side effects:
Eating disorders and substance abuse have many serious health consequences. The following is a list of potential side effects:
Anorexia
- Malnutrition
- Electrolyte imbalance
- Heart failure
- Reduction of bone density (osteoporosis)
- Kidney problems
- Hair loss
- Growth of a downy layer of hair all over the body (lanugo)
- In females, the absence of a period (amenorrhea)
- In males, decreased testosterone levels3,10
Bulimia
- Constipation
- Dehydration
- Missed periods or lack of menstrual periods
- Inflammation or rupture of esophagus
- Cavities and gum disease
- Ulcers
- Anemia
- Irregular heartbeat
- Heart failure
- Swollen cheeks (parotid salivary gland inflammation)6
Binge eating disorder
- Weight gain
- Anxiety
- Depression
- Obesity
- Type 2 diabetes
- High cholesterol levels
- Heart disease
- Gallbladder disease
- Joint pain
- Certain cancers
- Muscle pain3,8
Substance abuse (The long-term health consequences of substance abuse will vary depending on the type of drug being used and how it is used.)
- Cardiovascular disease
- Stroke
- Cancer
- HIV/AIDS
- Hepatitis
- Lung disease
- Mental disorders9
Symptoms
Below are lists of signs and symptoms of common eating disorders.
Anorexia
- Believing you are overweight when you are thin
- Fear of weight gain
- Refusal to eat
- Preoccupation with food
- Depression
- Compulsive exercise
- Withdrawal from family and friends
- Irritability
- Thoughts of suicide
- Extreme weight loss
- Hair thinning, breaking, or falling out
- Dry, yellowish skin
- Absence of menstruation
- Fluid collection/swelling in limbs (peripheral edema)4,10
Bulimia
- Preoccupation with your body shape and weight
- Living in fear of gaining weight
- Purging, or making yourself vomit after a binge
- Lack of control when binging
- Exercising despite poor weather, fatigue, or injury
- Eating to the point of pain
- Eating much more food in a binge than normal
- Using laxatives or diuretics to promote weight loss
- Using dietary supplements for weight loss6,11
Binge eating disorder
- Eating very large amounts of food over a short period of time (less than 2 hours)
- Feeling out of control while binging (unable to stop)
- Eating much faster than normal
- Eating large amounts when not hungry
- Secretive eating behavior (eating alone or in the car, hiding wrappers, hoarding food)
- Feelings of worthlessness, shame, or anger
- Feelings of disgust about body size7,12
Substance use disorder
- Feeling that you have to use the drug regularly (daily or even several times a day)
- Craving the drug
- Building tolerance, so that you need to take more of the drug to get the same effect
- Keeping a supply of the drug
- Spending money on the drug, even if you can’t afford it
- Failing to meet obligations and work responsibilities
- Stealing or doing things you wouldn’t normally do to get the drug
- Driving or engaging in other risky activities while high
- Spending more time and energy on getting and using the drug
- Being unable to stop using the drug
- Experiencing withdrawal symptoms when you try to stop taking the drug13
Causes
There is no single cause for either substance abuse or eating disorders. Instead, both are believed to be caused by a combination of biological, genetic, social, and environmental factors. These can include any of the following:4,14
- Family history of eating disorders or substance abuse
- Brain chemistry
- Media-promulgated societal norms/cultural pressure
- Low self-esteem
- Mental health issues, such as obsessive-compulsive disorder (OCD), anxiety, mood disorders, and personality disorders
- History of abuse or trauma
- Environment, including family attitudes toward drugs and peer groups that encourage drug use
- Genetics
Treatment at Dual Diagnosis Recovery Centers
 If you or someone you love is suffering from an eating disorder and a substance use disorder, you will need to look for specialized help. There are many treatment programs that simultaneously treat both disorders for optimal recovery chances.
If you or someone you love is suffering from an eating disorder and a substance use disorder, you will need to look for specialized help. There are many treatment programs that simultaneously treat both disorders for optimal recovery chances.
Dual diagnosis treatment programs can be inpatient or outpatient. Doctors or other health professionals evaluate patients to determine their particular addiction and their medical and psychiatric needs. These programs may use a combination of medication and behavioral therapies to facilitate recovery.
Some people struggling with severe malnutrition need medical care to strengthen their bodies before detox.
Treatment for addiction usually begins with a period of detoxification. An initial medical evaluation will assess the need for medical intervention and detox monitoring. For example, some people struggling with severe malnutrition need medical care to strengthen their bodies before detox. After detox, patients will begin individual and group therapy, which involves building skills to identify triggers and make healthier decisions. It may involve individual, group, and family therapy, along with 12-step meetings, medications, and aftercare planning.
The following are common treatments for eating disorders:
Anorexia
- Treatment for anorexia usually includes psychotherapy, family therapy, medication, and nutritional counseling.
- Some people arrive with severe malnutrition or a very low body mass index and may require constant medical monitoring in a hospital-like setting. This could include IV treatments.4
Bulimia
- In a residential treatment center, patients can benefit from 24/7 medical care, therapy, and nutritional education. Inpatient is usually a good fit for patients who do not have serious medical complications but still have psychiatric problems and are not ready for outpatient treatment.
- Outpatient programs are similar, combining cognitive behavioral therapy (CBT), group counseling, and medications.
- Doctors often prescribe antidepressant medication, such as the selective serotonin reuptake inhibitors (SSRIs) Lexapro, Prozac, and Zoloft.
- Support groups may be helpful for people with mild conditions and no health problems.4
Binge eating disorder
- Treatment for binge eating resembles that of bulimia and can be done on an inpatient or outpatient basis. Individual and group therapy will be combined with antidepressants and nutritional management.
- Many people with binge eating disorder are obese, so treatment often involves a weight loss or diet management plan.4
Sources
- National Institute on Drug Abuse. (2011). What is comorbidity?
- National Eating Disorders Association. What are eating disorders?
- The National Center on Addiction and Substance Abuse at Columbia University. (2003). Food for thought: Substance abuse and eating disorders.
- University of Maryland Medical Center. (2013). Eating disorders.
- National Eating Disorders Association. Anorexia nervosa.
- U.S. Department of Health and Human Services. (2012). Bulimia nervosa fact sheet.
- National Eating Disorders Association. Binge eating disorder.
- National Institute of Diabetes and Digestive and Kidney Diseases. (2016). Definition and facts for binge eating disorder.
- National Institute on Drug Abuse. (2017). Health consequences of drug misuse.
- The Mayo Clinic. (2016). Anorexia nervosa.
- Mayo Clinic. (2016.) Bulimia nervosa.
- Mayo Clinic. (2016). Binge eating disorder.
- Mayo Clinic. (2012). Drug addiction: Symptoms.
- Mayo Clinic. (2012). Drug addiction: Causes.
